What is Trichotillomania?
People with trichotillomania pull their hair out, usually from the scalp, eyebrows or eyelashes, but it can affect any hair on their body. They often do this unconsciously and are not aware they’re doing it.
The urge to pull is triggered by an emotional or physical feeling, like an itch or tingle. It’s followed by a brief sense of relief and becomes a habit.
Causes
The cause of trichotillomania isn’t known, but it is likely to be a combination of genetic and environmental factors. Trichotillomania tends to run in families, and a family member who has the disorder may increase your risk of getting it yourself. Certain mutations in the SLITRK1, 5HT2A, SAPAP3 and HOXB8 genes have been associated with trichotillomania. The condition also seems to occur more frequently among people who have a history of depression or anxiety disorders.
Trichotillomania can affect men and women of any age, although it’s more common in young children and adolescents. The hair-pulling disorder usually starts before or during the early teens, between ages 10 and 13 years, but it can continue to be a problem throughout adulthood. Trichotillomania may occur on its own or in conjunction with other mental health conditions such as bulimia, obsessive-compulsive disorder (OCD), and body dysmorphic disorder.
The disorder can be divided into two types: automatic pulling and focused pulling. People with automatic trichotillomania often pull their hair without realizing it, such as when they’re watching TV or reading. Those with focused trichotillomania tend to wait until they’re alone and then pull their hair very deliberately. People with the disorder may also be compelled to chew their nails or pick at their skin, and they may try to hide their behavior by wearing hats, scarves or false eyelashes and eyebrows.
Constant hair-pulling can damage your hair, which can lead to bald patches or thinning hair. It can also damage your skin, causing redness and scarring. In addition, those who eat their pulled hair may develop large hair balls (trichobezoars) in the digestive tract, which can cause weight loss, vomiting and even intestinal obstruction.
Many people with trichotillomania hide their symptoms, afraid they’ll be stigmatized or not taken seriously by medical professionals. However, trichotillomania is a recognized mental illness, and people who have it should be encouraged to seek help.
Talking to your doctor about trichotillomania is an important step in getting treatment, as the disorder can have a significant impact on your life and well-being. Some healthcare providers may refer you to a psychiatrist or other mental health provider for an interview about your symptoms. Many people with trichotillomania find relief from opening up about their condition to friends and family members. They can also find support through online communities such as Trichotillomania Support. There are no medications approved for trichotillomania, but selective serotonin reuptake inhibitors (SSRIs), antidepressants and other medicines used to treat anxiety and depression can help some people who have the condition.
Symptoms
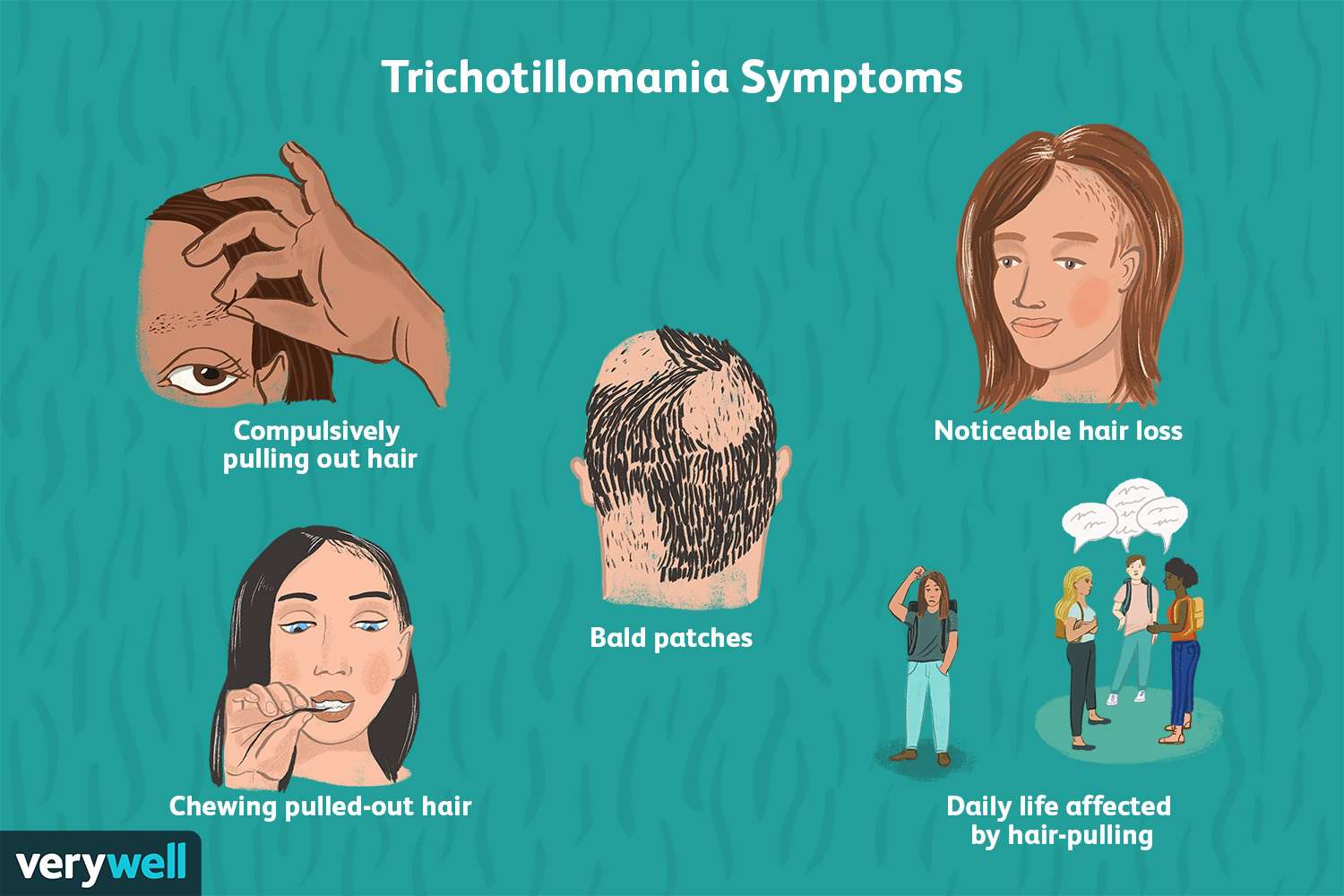
People with trichotillomania have a strong, irresistible urge to pull out their hair from the scalp, eyebrows, eyelashes, arms or pubic area. This results in patchy bald or thin spots and causes distress and shame. The condition can be long-term, and symptoms may come and go. In some cases, it may cause so much distress that a person avoids social and work functions or wears hats or wigs.
The disorder is most common in girls and boys age 8 to 12. It tends to occur during puberty. Often, kids with trichotillomania are secretive about their hair pulling and try to hide it from others. This can cause them to get teased or picked on for their appearance and lead to low self-esteem. The condition can also lead to depression and anxiety disorders.
A child who has trichotillomania will have trouble stopping the behavior even when it is causing significant distress. They may try to resist the impulse by putting their hands in their pockets, chewing their lips or biting their nails, but the urge will usually win out. In addition, the constant tugging can cause skin and hair damage. This can leave scars and affect the growth of hair over time, or even cause permanent baldness. It can also create thick, matted wads of hair called trichobezoars that can clog the digestive tract and cause gastrointestinal pain and discomfort.
There is no single cause for trichotillomania, although some studies suggest a link to genes. Other researchers believe that stressful life events can trigger it. People who have trichotillomania also often have anxiety or other mental health disorders such as depression, bipolar disorder or obsessive compulsive disorder (OCD).
Children with the condition can be treated by a psychiatrist or therapist. During treatment, they will learn techniques to help them manage their emotions and overcome the impulse to pull hair. They will work with the therapist to understand whether their hair pulling is automatic or focused, and they will practice replacing it with other behaviors. They may also take medication to reduce their anxiety.
It’s important to find a healthcare provider who is familiar with trichotillomania and can offer you the best care. You may need to see several specialists to get diagnosed and receive treatment. These specialists can include a dermatologist, a psychiatrist and a psychologist. They can treat the condition using cognitive behavioral therapy or habit reversal training, as well as medications to reduce anxiety.
Treatment
Trichotillomania is a chronic condition that requires lifelong treatment. There are a variety of treatments available for the disorder, including medication and psychotherapy. Some medications may help relieve the symptoms of trichotillomania, while others can also help reduce anxiety and depression. Psychotherapy can teach you to cope with your urges and manage your condition more effectively. The most common symptom of trichotillomania is compulsive hair pulling, which can result in noticeable and often irregularly-shaped patches of baldness on the scalp and other body parts, such as eyelashes and eyebrows. People with trichotillomania also commonly have other body-focused repetitive behaviors, such as chewing or eating their hair.
Getting the right treatment for trichotillomania is crucial for improving your quality of life. The first step is to find a mental health professional with experience treating this condition. Choosing someone with specialized training in behavioral therapies, such as habit reversal therapy, is especially important.
The most effective way to treat trichotillomania is with therapy, particularly cognitive behavior therapy (CBT). This type of therapy can teach you to recognize your urges and use techniques to manage them, such as refocusing your attention or using a reward system to prevent you from acting on your urges. CBT can also be used to address underlying psychological or emotional problems that might be contributing to your trichotillomania.
Many people with trichotillomania report that they feel a tension or an urge to pull their hair, which can be triggered by boredom, stress or even anger. They may also feel relief or pleasure during or after a hair-pulling session.
Some research suggests that trichotillomania is linked to serotonin, an enzyme that controls moods. This is why some people with the condition have a family history of depression or other mental health conditions, and why childhood trauma can contribute to the development of trichotillomania.
There are a number of medications that can be used to treat the symptoms of trichotillomania, including antidepressants and some types of antipsychotics. Some medications, such as the tricyclic antidepressant clomipramine (Anafranil), can reduce the severity of trichotillomania. Other medications, such as naltrexone (Reviax), which stops opioids from binding to brain receptors, have shown promise for treating some trichotillomania patients.
Prevention
Hair pulling can be a serious and debilitating condition, especially for those who are self-conscious about their appearance. People with trichotillomania often feel trapped in a cycle of compulsive behavior they can’t control. They may be hard on themselves and blame themselves for the problem, while family and friends struggle to understand what they’re going through. Some people with trichotillomania also feel embarrassed about their condition, leading them to avoid social activities and turn down job opportunities for fear of being found out. Others may try to hide their condition by wearing wigs or using make up to conceal bald spots.
Trichotillomania can affect any hair on the body, but most people who have the disorder pull from the head. It typically starts in adolescence and can last for several years through adulthood. Men and women are equally affected, though females can experience a more severe form of the condition during menstruation.
Genetics and childhood trauma may be risk factors for trichotillomania, and many people who have this disorder also have other mental health conditions like anxiety and depression. Trichotillomania can also be triggered by stressful events and situations, such as losing a loved one or being involved in a car accident.
Treatment options for trichotillomania include behavioral therapy, which is the most effective way to manage the disorder. This type of treatment involves working with a professional who can help you learn to recognize the triggers and urges for pulling, and find ways to cope with them. This can be done in a group setting with other people who have trichotillomania, or in individual therapy sessions.
There are also medications that can be used to reduce the frequency of urges to pull, though these should only be used under a doctor’s care. Using these medications too frequently can increase your risk for side effects, such as dizziness and blurred vision.
If you have trichotillomania, you should seek help from your doctor or a mental health professional right away. They can help you get treatment that can help you overcome the problem and live a full life. They might refer you to a specialist who can help you with trichotillomania, or they may recommend other treatments that can help you stop your hair-pulling habits, such as habit reversal therapy and cognitive therapy.





